Femoroacetabular Impingement Hip (FAI) vs Hip Flexor Strain - Self Tests
Are you feeling pain in your groin? If so, you may be suffering from either Hip Impingement (FAI) or Hip Flexor Strain. In this video, we'll show you how to do a self test to determine which injury you have.
If you're suffering from pain in your groin, don't wait to see a doctor. Instead, try doing a self test to determine whether you have Hip Impingement (FAI) or Hip Flexor Strain. This test is quick and easy and can help you get the care you need to recover and heal!
Want more info?
Option 1: Groin On-Demand Webinar https://bit.ly/37thtNF
Option 2: Video Guide https://bit.ly/33aLIqC
Option 3 (the best): Work With Us https://www.p2sportscare.com/
To work with us, contact us using this link https://bit.ly/3zCBnzZ or call us 714-502-4243. We have online programs, virtual and in-person options.
Costa Mesa, CA www.p2sportscare.com
[Performance Place website low back article excerpt] Hip flexor pain can wreak havoc on your love for running. Many of us run for weight loss or because it’s something we feel we “need to do” to be healthy. But not Julie. She simply loved the act of running!
A 10-minute marathon runner in her mid-40s, Julie would typically run five days per week. Some days she would run in track groups, rising to the challenge when her friends motivated her to get faster. Other times, she relished the solitude of solo runs.
Running was Julie’s “fix.” So when a cluster of symptoms started keeping her from doing what she loved, she knew she needed to take action. She came to Performance Place® Sports Care after seven months of unsuccessful attempts at treating the pain. I knew a detailed examination and proper guidance on how to decrease her symptoms would get her on the right track.
How It All Started
About 10 months ago, Julie began to notice hip flexor and sit bone pain when she ran. Since she didn’t do anything to create it, she thought it would go away on its own—just like most of her minor running-related issues had in the past.
But this time was different.
Soon, her hip flexor and sit bone were starting to ache at the very first step of her morning run, causing her pain for the entire duration. Her sit bone region would feel aggravated all day, especially exacerbated when she sat for long periods of time at work. The pain weighed on Julie’s mind. She wondered what she could do to make it go away.
When Julie couldn’t stand the aching any longer, she decided to take a break from running for a few days. Her hip flexor pain stopped, so she made the difficult decision of not running for two weeks.
Although it was painful to give up running, she hoped the pause would give the condition time to improve. And it did—until she hit the track again.
Just one minute into Julie’s first run in weeks, the pain surged back in full force. Frustrated, she decided to seek help.
What Didn’t Work
Julie started by exploring the typical healthcare route. But she quickly became irritated when her primary care doctor suggested rest and over-the-counter anti-inflammatory medications. She had already tried rest, to no avail, and she didn’t like the idea of medication. Her doctors thought she could have a labral tear in her hip, hip impingement or hip arthritis.
Unsatisfied, Julie searched for a better solution.
Her next stop was to see a physical therapist who was highly recommended by one of her friends. Physical therapy was covered by Julie’s insurance, minus deductible and copay, so she decided to give it a try.
Under her physical therapist’s guidance, Julie tried to remedy her problems with a daily 15-minute routine consisting of stretching, glute strengthening and hip mobility drills. As her inpatient care, she received tool-assisted soft tissue work. But despite two months of diligently following this plan, her sit bone was still tender while sitting at work. And she still hadn’t returned to running.
Frustrated by the lack of progress, Julie continued searching for a real solution.
Next, she visited a chiropractor suggested by a friend whose sciatica and hip pain had improved under his care. Julie received adjustments and soft tissue work two times per week, which was covered partially by her insurance. But after three months, she saw little improvement.
At this point, Julie was beyond frustrated. It had been five months since she was able to run, and there was still no real solution in sight. She decided to search the Runner’s World forum for more ideas on how to loosen up her hip flexor. After learning about the Active Release Technique, she visited a specialist who cost $150 per 15-minute session—not a penny covered by her insurance. After two months, the treatment yielded no improvement.
#FemoroacetabularImpingementvsHipFlexorStrain #femoralacetabularimpingement #california
21
views
How To Stretch A Pectineus Muscle Strain For Pain Relief
If you're experiencing pain in the front of you hip or groin, you may have a Pectineus muscle strain. We'll show you how to stretch the Pectineus muscle strain and relieve your pain.
This Pectineus muscle strain stretch is a great way to prevent further damage to the muscle and to speed the healing process. After you've done the stretch, be sure to apply heat to the area to help heal the muscle faster. If you follow these steps, you'll be able to get relief from your Pectineus muscle strain and keep your hip and adductor healthy!
Want more info? We have a free webinar that covers hip joints, labrums, groin, adductor, lower abdominal strains and sports hernia diagnosis in detail. Use this link to get access.
Option 1: Groin On-Demand Webinar https://www.p2sportscare.com/webinars/#flexor
Option 2: Self Help eBooks https://www.p2sportscare.com/product/understanding-hip-diagnosis-book/ and https://www.p2sportscare.com/product/weight-training-back-hip-groin/
Option 3: 12 Week Video Guide https://www.p2sportscare.com/product/hip-program/
Option 4 (the best): Work With Us https://www.p2sportscare.com/
[Performance Place website low back article excerpt] Hip flexor pain can wreak havoc on your love for running. Many of us run for weight loss or because it’s something we feel we “need to do” to be healthy. But not Julie. She simply loved the act of running!
A 10-minute marathon runner in her mid-40s, Julie would typically run five days per week. Some days she would run in track groups, rising to the challenge when her friends motivated her to get faster. Other times, she relished the solitude of solo runs.
Running was Julie’s “fix.” So when a cluster of symptoms started keeping her from doing what she loved, she knew she needed to take action. She came to Performance Place® Sports Care after seven months of unsuccessful attempts at treating the pain. I knew a detailed examination and proper guidance on how to decrease her symptoms would get her on the right track.
How It All Started
About 10 months ago, Julie began to notice hip flexor and sit bone pain when she ran. Since she didn’t do anything to create it, she thought it would go away on its own—just like most of her minor running-related issues had in the past.
But this time was different.
Soon, her hip flexor and sit bone were starting to ache at the very first step of her morning run, causing her pain for the entire duration. Her sit bone region would feel aggravated all day, especially exacerbated when she sat for long periods of time at work. The pain weighed on Julie’s mind. She wondered what she could do to make it go away.
When Julie couldn’t stand the aching any longer, she decided to take a break from running for a few days. Her hip flexor pain stopped, so she made the difficult decision of not running for two weeks.
Although it was painful to give up running, she hoped the pause would give the condition time to improve. And it did—until she hit the track again.
Just one minute into Julie’s first run in weeks, the pain surged back in full force. Frustrated, she decided to seek help.
What Didn’t Work
Julie started by exploring the typical healthcare route. But she quickly became irritated when her primary care doctor suggested rest and over-the-counter anti-inflammatory medications. She had already tried rest, to no avail, and she didn’t like the idea of medication. Her doctors thought she could have a labral tear in her hip, hip impingement or hip arthritis.
Unsatisfied, Julie searched for a better solution.
Her next stop was to see a physical therapist who was highly recommended by one of her friends. Physical therapy was covered by Julie’s insurance, minus deductible and copay, so she decided to give it a try.
Under her physical therapist’s guidance, Julie tried to remedy her problems with a daily 15-minute routine consisting of stretching, glute strengthening and hip mobility drills. As her inpatient care, she received tool-assisted soft tissue work. But despite two months of diligently following this plan, her sit bone was still tender while sitting at work. And she still hadn’t returned to running.
Frustrated by the lack of progress, Julie continued searching for a real solution.
Next, she visited a chiropractor suggested by a friend whose sciatica and hip pain had improved under his care. Julie received adjustments and soft tissue work two times per week, which was covered partially by her insurance. But after three months, she saw little improvement.
#StretchAPectineusMuscleStrain #PainRelief
16
views
How to Perform A Rhomboid Pain Release (TRY IT)
How to Perform A Rhomboid Release (TRY IT)
714-502-4243 | Costa Mesa, CA | http://www.p2sportscare.com
FREE TIPS AUDIO DOWNLOAD - https://bit.ly/3kvbqfJ
Complete 4 Week Web-based Shoulder Rehab Guide: https://bit.ly/3hNsAB9
We have received countless requests for exercises for shoulder blade and upper trap pain, so we created an affordable 4 week guide you can do from home.
If the test in this video worked for you, then this guide might just be your best friend! https://bit.ly/3hNsAB9
If you're local, come see us in Costa Mesa, CA.
Shoulder blade pain can feel like aches/spasms of muscles under the shoulder blade and are often confused as being muscle knots or trigger points. Shoulder blade pain is treatable with exercise therapy, in combination with manual therapy. Often times resolving in weeks to months, depending upon severity.
When we wrote this description, we decided to interview a few people just like you who’ve had shoulder blade pain. They were nice enough to share their stories so we can learn from them.
Case #1
The most enlightening of the interviews was Becky.
She was able to successfully return to full activity (work, yoga, and sleep) after suffering from shoulder blade pain just like you.
Becky has been a nurse for the past 10 years. She works 5 days a week in the hospital, moving patients, charting notes, and educating her patients about how to live a healthy life.
She’s now fully capable of rolling patients over in bed, pushing wheelchairs, and going throughout her day without neck, shoulder blade or arm pain. Sleeps like the dead at night without the assistance of medication of any kind.
But she didn’t always feel this good…
10 years ago, Becky was in grad school when she started to develop light headaches. Most days were mild just a light throbbing ache around the base of her head. Other days her headache would wrap around her head, towards her eyes and travel downward towards her shoulders. She got through most of the day with the help of a frequent self-massage and bi-weekly chiropractic work.
A few years later, her symptoms began to evolve.
Even though she feels great today, she can still recall the details like it was yesterday.
Most days she was in intense pain from the moment she opened her eyes in the morning. Sleeping was terrible due to the fact that it felt like someone was taking a hand drill and boring a hole into her right arm bone all night, directly through her bicep.
Throughout the day, her pain began to increase and creep down into her midback and upper trap area. The pain was so intense at times that she said she would have been “willing to cut her arm off” if it would take the pain away.
She had to stop doing yoga, was unable to sleep at night and considered quitting her job.
Tucking her chin and looking upward at the sky was painful. Looking down to her chest was much better, but still not pain-free. While driving, she could not turn her head to check for cars as she changed lanes. She even bought those little blindspot mirrors so she could safely change lanes.
Sounds intense right? Yet, she was able to overcome it.
What did she do to feel better?
She didn’t get better overnight. She spent months having her neck adjusted and getting massages with very temporary relief.
Eventually, she found a chiropractor specializing in focal soft tissue work help her release a nerve in her neck and shoulder. After that, she began to progressively get better. She looked forward to being able to work without pain and more importantly sleep and do yoga without any issues.
Want to be like Becky?
You can, you just need the correct plan of attack. The human body is truly resilient. You are just as resilient.
What is the correct plan of attack for shoulder blade pain?
Recovery is simple if we first address the red herring that tends to distract people away from REAL recovery.
REAL recovery returns you to ALL of the sports and hobbies that you love. Avoiding them because you feel “you’re getting too old” or afraid the pain will return is the wrong approach.
Ask yourself what REAL recovery is for you.
What activity would you return to if you had ZERO fear of your shoulder blade pain returning?
Set a goal and focus on it. Set your goals high.
Do you want to rock climb?
Carry your daughter around on your shoulder?
Play baseball and even pitch?!
This article will help you get there!
But first let’s get back to that red herring…
Companies that sell foam rollers, massagers, and trigger point products want you to believe your mid back/ shoulder blade pain is from a knotted up muscle, but they are wrong.
You simply need to address the root cause, and that can be done through movement exercises such as this chin tuck. We've got that and a 4 week plan to help you start your recovery. It's easy to do from anywhere, and affordable. Get it here: https://bit.ly/3hNsAB9
#RhomboidPainRelease #california #chiropractic
16
views
How to Fix Lower Back Strain (DON'T STRETCH)
How to Fix Lower Back Strain (DON'T STRETCH)
714-502-4243 Costa Mesa CA
http://www.p2sportscare.com
FREE gift! Low back webinar: https://bit.ly/3qIPhvU
#lowbackstrain #lowerback #lowbackpain
Low back pain and strain is common in people over the age of 30. It does not have to be the end of your life. Most people recovery from a lower back strain... they just need to know how to fix it.
Low back herniations, or lumbar herniations, are a very common injury we "fix" at Performance Place. These injuries tend to follow similar patterns, and so we have decided to share two of the most common things that can help alleviate disc pain instantly.
Doctors Dawne and Sebastian spend some time talking about whether you can "fix" a disc or not, and what part MRI and imaging has to play in your recovery. They demonstrate a breathing position and technique that corresponds with a position of relief for the low back, which can help immediately. They also demonstrate low back extension and its importance in relieving pain associated with low back disc herniations. Get your here!
For other helpful videos:
Is Walking Good for a Disc Herniation?
https://www.youtube.com/watch?v=nDA-8OEKf1E&t=2s
Can a Herniated Disc Fix Itself?
https://www.youtube.com/watch?v=Iuvt_WbKwZ8&t=169s
Can a Chiropractor Help You Fix a Disc Herniation?
https://www.youtube.com/watch?v=KRzxBzgaq4k&t=4s
What is a Disc Herniation?
https://www.youtube.com/watch?v=wFvTIzePgQQ&t=1s
Dr. Gonzales is a Costa Mesa chiropractor serving Costa Mesa and Huntington Beach and the surrounding community. Regardless if you are suffering from back pain, neck pain, headaches, shoulder pain, or sports injuries, our chiropractor can help you heal your conditions with chiropractic treatments and massage, such as Active Release. If you have been in a car accident, there is a chance you need a Chiropractor in Costa Mesa to help you overcome conditions, which occur in car accidents, such as whiplash. Dr. Gonzales, who has been a Costa Mesa Chiropractor for runners, triathletes and golfers can help you with chronic conditions as well as acute sports injuries. Visit our website and book a free consultation to see our chiropractor for chiropractic care today.
Never been to a chiropractor before? No worries! The first session to our Chiropractic Center in Costa Mesa will consist of a consultation with one of our chiropractors, where we will perform treatment on the very same day... you'll feel pain relief before you leave our chiropractic sports center. Our team of therapists and doctors are honest and will help you decided the right treatment plan for you.
How long will my care be at a Chiropractic Clinic? Every chiropractic clinic is different but our chiropractors in Costa Mesa have been known for providing short treatment plans and keeping Huntington Beach's active community moving with minimal downtime.
Different people suffer through different health disorders that need to have several doctors and medical practitioners who can get them rid from their problems. In this way, Chiropractor is available for all these purposes. It is the health care medical facility that provides instant relief against all kinds of problems.
Chiropractic is a natural healing science, art and philosophy primarily concerned with detecting and then eliminating interference to your nervous system. Since your nervous system controls every aspect of your body, chiropractic can have a major impact on multiple areas of your health. Founded in 1895, it is the world's largest drug-free healthcare system and the 3rd largest primary healthcare system in the USA behind medicine and dentistry. Over 25 million Americans will see their chiropractor this year.
#HowtoFixLowerBackStrain #lowbackpainrelief #california
19
views
Must Know Sports Hernia Diagnosis Self Treatment/ Self Test
In this video, we show a sports hernia self treatment we give many of our clients. It is not the only part of treatment. Grabbing the skin around the region of the groin strain can reduce pain and stiffness with turning and twisting. Sports hernias are often misdiagnosed with hip labrum tears, hip impingement, adductor tendonitis and abdominal strains.
Option 1: Groin On-Demand Webinar https://bit.ly/37thtNF
Option 2: eBook Unveiling The Mystery Behind Groin Pain in Athletes https://www.p2sportscare.com/product/understanding-sports-hernias-unveiling-the-mystery-behind-groin-pain/
Option 2: Video Guide https://bit.ly/33aLIqC
Option 3 (the best): Work With Us https://www.p2sportscare.com/
Sports Hernia Diagnosis
What Is A Sports Hernia?
A sports hernia is tearing of the transversalis fascia of the lower abdominal or groin region. A common misconception is that a sports hernia is the same as a traditional hernia. The mechanism of injury is rapid twisting and change of direction within sports, such as football, basketball, soccer and hockey.
The term “sports hernia” is becoming mainstream with more professional athletes being diagnosed. The following are just to name a few:
Torii Hunter
Tom Brady
Ryan Getzlaf
Julio Jones
Jeremy Shockey
If you follow any of these professional athletes, they all seem to have the same thing in common: Lingering groin pain. If you play fantasy sports, this is a major headache since it seems so minor, but it can land a player on Injury Reserve on a moments notice. In real life, it is a very frustrating condition to say the least. It is hard to pin point, goes away with rest and comes back after activity, but is hardly painful enough to make you want to stop. It lingers and is always on your mind. And if you’re looking for my step-by-step sports hernia rehab video course here it is.
One the best definitions of Sport hernias is the following by Harmon:
The phenomena of chronic activity–related groin pain that it is unresponsive to conservative therapy and significantly improves with surgical repair.”
This is truly how sports hernias behave in a clinical setting. It is not uncommon for a sports hernia to be unrecognized for months and even years. Unlike your typical sports injury, most sports medicine offices have only seen a handful of cases. It’s just not on most doctors’ radar. The purpose of this article is not only to bring awareness about sports hernias, but also to educate.
Will you find quick fixes in this article for sports hernia rehab?
Nope. There is no quick fix for this condition, and if someone is trying to sell you one, they are blowing smoke up your you-know-what.
Is there a way to decrease the pain related to sports hernias?
Yes. Proper rehab and avoidance of activity for a certain period of time will assist greatly, but this will not always stop it from coming back. Pain is the first thing to go and last thing to come. Do not be fooled when you become pain-free by resting it. Pain is only one measure of improvement in your rehab. Strength, change of direction, balance and power (just to name a few) are important, since you obviously desire to play your sport again. If you wanted to be a couch potato, you would be feeling better in no time. Watching Sports Center doesn’t require any movement.
Why is this article so long?
There is a lot of information on sports hernias available to you on the web. However, much of the information is spread out all over the internet and hard for athletes to digest due to complicated terminology. This article lays out the foundational terminology you will need to understand what options you have with your injury. We will go over anatomy, biomechanics, rehab, surgery, and even the fun facts. The information I am using is from the last ten years of medical research, up until 2016. We will be making updates overtime when something new is found as well. So link to this page and share with friends. This is the best source for information on sports hernias you will find.
Common Names (or Aliases?) for Sports Hernias
Sportsman’s Hernia
Athletic Pubalgia
Gilmore’s Groin
How Do You Know If You Have A Sports Hernia?
Typical athlete characteristics:
Male, age mid-20s
#sportsherniadiagnosisselftreatment #sportshernia #california
13
views
3 Best Groin Pain Treatments: Anyone With Adductor Hip Pain Should Try These!
Groin Pain? Try these three best groin pain treatments! If you're suffering from groin pain, you don't have to live with it. In this video, we'll share with you three best groin pain treatments that you can try. We show a groin stretch and a physical therapy technique to increase hip mobility. These treatments will help you get relief from your pain fast!
Want more info?
Option 1: Groin On-Demand Webinar https://bit.ly/37thtNF
Option 2: Video Guide https://bit.ly/33aLIqC
Option 3 (the best): Work With Us https://www.p2sportscare.com/
#GroinPainTreatments #AdductorHipPain #hippain
To work with us, contact us using this link https://bit.ly/3zCBnzZ or call us 714-502-4243. We have online programs, virtual and in-person options.
Costa Mesa, CA www.p2sportscare.com
[Performance Place website low back article excerpt] Hip flexor pain can wreak havoc on your love for running. Many of us run for weight loss or because it’s something we feel we “need to do” to be healthy. But not Julie. She simply loved the act of running!
A 10-minute marathon runner in her mid-40s, Julie would typically run five days per week. Some days she would run in track groups, rising to the challenge when her friends motivated her to get faster. Other times, she relished the solitude of solo runs.
Running was Julie’s “fix.” So when a cluster of symptoms started keeping her from doing what she loved, she knew she needed to take action. She came to Performance Place® Sports Care after seven months of unsuccessful attempts at treating the pain. I knew a detailed examination and proper guidance on how to decrease her symptoms would get her on the right track.
How It All Started
About 10 months ago, Julie began to notice hip flexor and sit bone pain when she ran. Since she didn’t do anything to create it, she thought it would go away on its own—just like most of her minor running-related issues had in the past.
But this time was different.
Soon, her hip flexor and sit bone were starting to ache at the very first step of her morning run, causing her pain for the entire duration. Her sit bone region would feel aggravated all day, especially exacerbated when she sat for long periods of time at work. The pain weighed on Julie’s mind. She wondered what she could do to make it go away.
When Julie couldn’t stand the aching any longer, she decided to take a break from running for a few days. Her hip flexor pain stopped, so she made the difficult decision of not running for two weeks.
Although it was painful to give up running, she hoped the pause would give the condition time to improve. And it did—until she hit the track again.
Just one minute into Julie’s first run in weeks, the pain surged back in full force. Frustrated, she decided to seek help.
What Didn’t Work
Julie started by exploring the typical healthcare route. But she quickly became irritated when her primary care doctor suggested rest and over-the-counter anti-inflammatory medications. She had already tried rest, to no avail, and she didn’t like the idea of medication. Her doctors thought she could have a labral tear in her hip, hip impingement or hip arthritis.
Unsatisfied, Julie searched for a better solution.
Her next stop was to see a physical therapist who was highly recommended by one of her friends. Physical therapy was covered by Julie’s insurance, minus deductible and copay, so she decided to give it a try.
Under her physical therapist’s guidance, Julie tried to remedy her problems with a daily 15-minute routine consisting of stretching, glute strengthening and hip mobility drills. As her inpatient care, she received tool-assisted soft tissue work. But despite two months of diligently following this plan, her sit bone was still tender while sitting at work. And she still hadn’t returned to running.
Frustrated by the lack of progress, Julie continued searching for a real solution.
Next, she visited a chiropractor suggested by a friend whose sciatica and hip pain had improved under his care. Julie received adjustments and soft tissue work two times per week, which was covered partially by her insurance. But after three months, she saw little improvement.
At this point, Julie was beyond frustrated. It had been five months since she was able to run, and there was still no real solution in sight. She decided to search the Runner’s World forum for more ideas on how to loosen up her hip flexor. After learning about the Active Release Technique, she visited a specialist who cost $150 per 15-minute session—not a penny covered by her insurance. After two months, the treatment yielded no improvement.
22
views
Top 3 Groin Pain Self Tests & Diagnosis Categories You Must Know 2024
In this video, we're going to be discussing the top 3 groin pain self tests and diagnosis. We'll be discussing the cause of groin pain, the various types of groin pain, and the best way to treat them.
If you're suffering from groin pain and don't know what it is, this video is for you! We'll discuss the top 3 groin pain self tests and diagnosis and help you find the best treatment for your specific case. So don't wait! Watch this video and find out how to treat your Groin Pain right away!
Want more info?
Option 1: Groin On-Demand Webinar https://www.p2sportscare.com/webinars/#flexor
Option 2: 12 Week Video Guide https://www.p2sportscare.com/product/hip-program/
Option 3 (the best): Work With Us https://www.p2sportscare.com/
To work with us, contact us using this link https://www.p2sportscare.com/contact-form-youtube/ or call us 714-502-4243. We have online programs, virtual and in-person options.
Costa Mesa, CA www.p2sportscare.com
[Performance Place website low back article excerpt] Hip flexor pain can wreak havoc on your love for running. Many of us run for weight loss or because it’s something we feel we “need to do” to be healthy. But not Julie. She simply loved the act of running!
A 10-minute marathon runner in her mid-40s, Julie would typically run five days per week. Some days she would run in track groups, rising to the challenge when her friends motivated her to get faster. Other times, she relished the solitude of solo runs.
Running was Julie’s “fix.” So when a cluster of symptoms started keeping her from doing what she loved, she knew she needed to take action. She came to Performance Place® Sports Care after seven months of unsuccessful attempts at treating the pain. I knew a detailed examination and proper guidance on how to decrease her symptoms would get her on the right track.
How It All Started
About 10 months ago, Julie began to notice hip flexor and sit bone pain when she ran. Since she didn’t do anything to create it, she thought it would go away on its own—just like most of her minor running-related issues had in the past.
But this time was different.
Soon, her hip flexor and sit bone were starting to ache at the very first step of her morning run, causing her pain for the entire duration. Her sit bone region would feel aggravated all day, especially exacerbated when she sat for long periods of time at work. The pain weighed on Julie’s mind. She wondered what she could do to make it go away.
When Julie couldn’t stand the aching any longer, she decided to take a break from running for a few days. Her hip flexor pain stopped, so she made the difficult decision of not running for two weeks.
Although it was painful to give up running, she hoped the pause would give the condition time to improve. And it did—until she hit the track again.
0:00 Introduction
1:21 Hip Flexor Strain
2:23 Hip Impingement FAI
4:23 Spinal Referred Hip Pain
#GroinPainSelfTestsandDiagnosis #groinpain #california
8
views
Sports Hernia Vs. Groin Strain: An Engaging Discussion
In this video, we're going to be discussing the difference between a sports hernia and a Groin Strain. We'll also be giving you some tips on how to tell the difference and what to do if you experience either of these injuries.
If you're looking for advice on how to treat a Sports Hernia or Groin Strain, then this video is for you! We'll discuss the symptoms and treatment options for each injury, and help you make the right decision for your health. We hope you find this video helpful!
Option 1: Groin On-Demand Webinar https://bit.ly/37thtNF
Option 2: eBook Unveiling The Mystery Behind Groin Pain in Athletes https://www.p2sportscare.com/product/understanding-sports-hernias-unveiling-the-mystery-behind-groin-pain/
Option 3: Video Guide https://bit.ly/33aLIqC
Option 4 (the best): Work With Us https://www.p2sportscare.com/
#sportshernia #hernia #hippain
Sports Hernia Diagnosis
What Is A Sports Hernia?
A sports hernia is tearing of the transversalis fascia of the lower abdominal or groin region. A common misconception is that a sports hernia is the same as a traditional hernia. The mechanism of injury is rapid twisting and change of direction within sports, such as football, basketball, soccer and hockey.
The term “sports hernia” is becoming mainstream with more professional athletes being diagnosed. The following are just to name a few:
Torii Hunter
Tom Brady
Ryan Getzlaf
Julio Jones
Jeremy Shockey
If you follow any of these professional athletes, they all seem to have the same thing in common: Lingering groin pain. If you play fantasy sports, this is a major headache since it seems so minor, but it can land a player on Injury Reserve on a moments notice. In real life, it is a very frustrating condition to say the least. It is hard to pin point, goes away with rest and comes back after activity, but is hardly painful enough to make you want to stop. It lingers and is always on your mind. And if you’re looking for my step-by-step sports hernia rehab video course here it is.
One the best definitions of Sport hernias is the following by Harmon:
The phenomena of chronic activity–related groin pain that it is unresponsive to conservative therapy and significantly improves with surgical repair.”
This is truly how sports hernias behave in a clinical setting. It is not uncommon for a sports hernia to be unrecognized for months and even years. Unlike your typical sports injury, most sports medicine offices have only seen a handful of cases. It’s just not on most doctors’ radar. The purpose of this article is not only to bring awareness about sports hernias, but also to educate.
Will you find quick fixes in this article for sports hernia rehab?
Nope. There is no quick fix for this condition, and if someone is trying to sell you one, they are blowing smoke up your you-know-what.
Is there a way to decrease the pain related to sports hernias?
Yes. Proper rehab and avoidance of activity for a certain period of time will assist greatly, but this will not always stop it from coming back. Pain is the first thing to go and last thing to come. Do not be fooled when you become pain-free by resting it. Pain is only one measure of improvement in your rehab. Strength, change of direction, balance and power (just to name a few) are important, since you obviously desire to play your sport again. If you wanted to be a couch potato, you would be feeling better in no time. Watching Sports Center doesn’t require any movement.
Why is this article so long?
There is a lot of information on sports hernias available to you on the web. However, much of the information is spread out all over the internet and hard for athletes to digest due to complicated terminology. This article lays out the foundational terminology you will need to understand what options you have with your injury. We will go over anatomy, biomechanics, rehab, surgery, and even the fun facts. The information I am using is from the last ten years of medical research, up until 2016. We will be making updates overtime when something new is found as well. So link to this page and share with friends. This is the best source for information on sports hernias you will find.
Common Names (or Aliases?) for Sports Hernias
Sportsman’s Hernia
Athletic Pubalgia
Gilmore’s Groin
How Do You Know If You Have A Sports Hernia?
Typical athlete characteristics:
Male, age mid-20s
Common sports: soccer, hockey, tennis, football, field hockey
Motions involved: cutting, pivoting, kicking and sharp turns
Gradual onset
How A Sports Hernia Develops
Chronic groin pain typically happens over time, which is why with sports hernias, we do not hear many stories of feeling a “pop” or a specific moment of injury. It is the result of “overuse” mechanics stemming from a combination of inadequate strength and endurance, lack of dynamic control, movement pattern abnormalities, and discoordination of motion in the groin area.
#SportsHernia #GroinStrain
21
views
My 5 Favorite Ulnar Nerve Stretches - That Won't Hurt You
In this video we go over the 5 best Ulnar Nerve Stretches that don't have a high risk associated with them. Some ulnar nerve stretches can create more pain and numbness if you do them wrong. If you want more information about ulnar nerve recovery check out my ebook which covers, treatments, diagnosis, areas of entrapments, and mistakes. Go here: https://bit.ly/3hTNLlD
UPDATED VERSION OF THIS VIDEO: https://youtu.be/JWeP92auocE
If you would like some treatment call our office in Costa Mesa CA. We have virtual sessions as 714-502-4243 www.p2sportscare.com
CHAPTER 1: INTRODUCTION TO TREATING HAND NUMBNESS
Well, sorting through the treatment of hand numbness is a process, but that’s because of the variety of potential underlying causes for it which we have to review.
In this chapter, you’ll learn about the theory of how to comprehensively rehab and treat the symptoms of an ulnar nerve compression. HINT: This is the most important part for you to read.
Treatment of the ulnar nerve can be broken down into five parts:
Find the site of compression
Decrease local irritation (passively or actively)
Decrease activity creating compression (until under control)
Increase nerve’s ability to slide through
Improve postural control, breathing patterns, movement patterns, etc.
This will be worth your time. It’s only a 5 minute section before we go into the stretch and passive care you came to see.
1. Find the site of compression
Think of a nerve as a garden hose. Any kink in the hose will affect the water flow, regardless of its location. When considering ulnar nerve compression, it works much like the garden hose, but there are a few sites on the nerve that have high probability of becoming entrapped:
At the spine (the nerve root)
At the brachial plexus (the neck region)
At the brachial sleeve (the arm)
At the cubital tunnel (the elbow)
Within the forearm muscles
At the Tunnel of Guyon (the wrist)
There are also a few other underlying problems that can trigger “symptoms of an ulnar nerve compression.” Be warned, most of these are probably going to scare you; so seeing a doctor to confirm your specific cause is good prevention of unnecessary panic attacks.
I once had a patient experiencing numbness/pain in the ring and pinky fingers at night. In his case, the cause was a tumor in his spine.
Another young man came in and presented with bilateral (both sides) numbness and pain in his hands/fingers. This is one of the major signs (bilateral symptoms) of spinal cord compression.
The individuals involved in these cases both asked, “Hey, can you just treat it?” Of course, my answer was no. Cases like both of these must be referred out for further evaluation, treatment and care.
It’s sad and scary to hear horror stories like these, but the great news is if they are found early, then they can be corrected to some degree. Ignorance is only bliss for a period of time.
Moral of this story: you should know, with certainty, what is creating your symptoms. If you don’t, the muscles of the hand can end up wasting away, or even worse.
After we’ve screened out all the red flags, I often have my patients start to examine what changes their symptoms. To do this, I’ll have them keep all variables constant and only move ONE body region to a new position and hold it.
From center, does a tilt of the head to the opposite side increase or decrease symptoms?
From center, does dropping the chin to the chest change it?
How about a shoulder shrug?
Do you see what’s going on here? We are localizing the area that has the greatest effect on the hand numbness. Everyone is different, and sometimes it’s not a position change, but rather a “stiffening” of a region. We will get more into stabilization in the eBook.
2. Decrease local irritation
Decreasing irritation of the region of nerve compression can be helpful in decreasing “flare-ups.”
In most cases, people are pretty aware of what activities or motions will trigger their symptoms. I’m never one to encourage a mindset of “avoidance,” but in this case, while we attempt to fully address the reason for the nerve compression, holding off on those activities or motions might be a good idea.
If you’re thinking something along the lines of, “It happens when I drive. How can I not drive?” or some other activity that seems unlikely for you to stop entirely, then a little more effort is going to be necessary from you!
I strongly encourage my patients to break down every activity into its separate movements or components, and to find the EXACT reason for the flare-up. The more time we can get the nerve to “breathe freely”, the less inflammed it will be. It’s not always avoidance of an activity… most of the time it’s a simple modification.
#FavoriteUlnarNerveStretches #ulnarnervestretch #california
9
views
Can Low Back Pain Cause Groin Pain? Yes, Here's How
In this video, we will explain how can low back pain cause groin pain. Nerves and joints of the lower back can create groin or hip pain with referred pain. Pressing on muscles of the lower back or SI joint often sends pain traveling to the front of the hip. This groin/ hip pain can get worse with walking, picking up leg, running or getting into a car.
UPDATED VIDEO: https://youtu.be/djcvBfJS1Z0
Want more info? We have a free webinar that covers hip joints, labrums, groin, adductor, lower abdominal strains and sports hernia diagnosis in detail. Use this link to get access. https://bit.ly/37thtNF
To work with us, contact us using this link https://bit.ly/3zCBnzZ or call us 714-502-4243. We have online programs, virtual and in-person options.
Costa Mesa, CA www.p2sportscare.com
[Performance Place website low back article excerpt] Hip flexor pain can wreak havoc on your love for running. Many of us run for weight loss or because it’s something we feel we “need to do” to be healthy. But not Julie. She simply loved the act of running!
A 10-minute marathon runner in her mid-40s, Julie would typically run five days per week. Some days she would run in track groups, rising to the challenge when her friends motivated her to get faster. Other times, she relished the solitude of solo runs.
Running was Julie’s “fix.” So when a cluster of symptoms started keeping her from doing what she loved, she knew she needed to take action. She came to Performance Place® Sports Care after seven months of unsuccessful attempts at treating the pain. I knew a detailed examination and proper guidance on how to decrease her symptoms would get her on the right track.
How It All Started
About 10 months ago, Julie began to notice hip flexor and sit bone pain when she ran. Since she didn’t do anything to create it, she thought it would go away on its own—just like most of her minor running-related issues had in the past.
But this time was different.
Soon, her hip flexor and sit bone were starting to ache at the very first step of her morning run, causing her pain for the entire duration. Her sit bone region would feel aggravated all day, especially exacerbated when she sat for long periods of time at work. The pain weighed on Julie’s mind. She wondered what she could do to make it go away.
When Julie couldn’t stand the aching any longer, she decided to take a break from running for a few days. Her hip flexor pain stopped, so she made the difficult decision of not running for two weeks.
Although it was painful to give up running, she hoped the pause would give the condition time to improve. And it did—until she hit the track again.
Just one minute into Julie’s first run in weeks, the pain surged back in full force. Frustrated, she decided to seek help.
What Didn’t Work
Julie started by exploring the typical healthcare route. But she quickly became irritated when her primary care doctor suggested rest and over-the-counter anti-inflammatory medications. She had already tried rest, to no avail, and she didn’t like the idea of medication.
Unsatisfied, Julie searched for a better solution.
Her next stop was to see a physical therapist who was highly recommended by one of her friends. Physical therapy was covered by Julie’s insurance, minus deductible and copay, so she decided to give it a try.
Under her physical therapist’s guidance, Julie tried to remedy her problems with a daily 15-minute routine consisting of stretching, glute strengthening and hip mobility drills. As her inpatient care, she received tool-assisted soft tissue work. But despite two months of diligently following this plan, her sit bone was still tender while sitting at work. And she still hadn’t returned to running.
Frustrated by the lack of progress, Julie continued searching for a real solution.
Next, she visited a chiropractor suggested by a friend whose sciatica had improved under his care. Julie received adjustments and soft tissue work two times per week, which was covered partially by her insurance. But after three months, she saw little improvement.
At this point, Julie was beyond frustrated. It had been five months since she was able to run, and there was still no real solution in sight. She decided to search the Runner’s World forum for more ideas on how to loosen up her hip flexor. After learning about the Active Release Technique, she visited a specialist who cost $150 per 15-minute session—not a penny covered by her insurance. After two months, the treatment yielded no improvement.
In all, Julie’s seven months of health care had cost her more than $2500. But more critical than her financial hit was the void in her life from not running. She still couldn’t even jog without her hip flexor and sit bone immediately starting to ache.
#CanLowBackPainCauseGroinPain #groinpain #california
25
views
Groin Pulls (Adductor Strains) 9 Amazing Exercises & Stretches
In this video, we will show the Stretches & Exercises for Groin Pulls. This is a follow along video where we go through the whole home exercise and stretch program with you. We have stretches for the glute muscles, adductor muscles and hip capsule. We have strengthening exercises for the glute muscles, hip flexor, abs and legs.
Want more info? We have a free webinar that covers adductor strains, groin strains, hip joints, labrums, lower abdominal strains and sports hernia diagnosis in detail. Use this link to get access. https://bit.ly/37thtNF
#hippain #hipflexor #hipmobility
To work with us, contact us using this link https://bit.ly/3zCBnzZ or call us 714-502-4243. We have online programs, virtual and in-person options.
Costa Mesa, CA www.p2sportscare.com
An adductor muscle strain or groin pulls means the same thing. This diagnosis describes an injury to the junction of where the muscle becomes the tendon, also known as the musculotendinous junction.
A muscle strain is very different from a partial and complete muscles tear. Muscle tears tend to create local swelling AND bruising. Generally speaking if there was no bruising then there was not a large tear.
Partial tears mean the soft tissue is still attached to it’s proper location. In simple terms, there has been some tear
What does the diagnosis mean…. It is a symptom, not a diagnosis. Since it is a symptom, it is not describing WHY you are having the symptom and it does not identify a diagnosis.
Let me say this in simple terms: If your car doesn't start, it is a symptom. Possible reasons why or diagnoses would be: no battery, no starter, or you’re simply out of gasoline.
[Performance Place website low back article excerpt] Hip flexor pain can wreak havoc on your love for running. Many of us run for weight loss or because it’s something we feel we “need to do” to be healthy. But not Julie. She simply loved the act of running!
A 10-minute marathon runner in her mid-40s, Julie would typically run five days per week. Some days she would run in track groups, rising to the challenge when her friends motivated her to get faster. Other times, she relished the solitude of solo runs.
Running was Julie’s “fix.” So when a cluster of symptoms started keeping her from doing what she loved, she knew she needed to take action. She came to Performance Place® Sports Care after seven months of unsuccessful attempts at treating the pain. I knew a detailed examination and proper guidance on how to decrease her symptoms would get her on the right track.
How It All Started
About 10 months ago, Julie began to notice hip flexor and sit bone pain when she ran. Since she didn’t do anything to create it, she thought it would go away on its own—just like most of her minor running-related issues had in the past.
But this time was different.
Soon, her hip flexor and sit bone were starting to ache at the very first step of her morning run, causing her pain for the entire duration. Her sit bone region would feel aggravated all day, especially exacerbated when she sat for long periods of time at work. The pain weighed on Julie’s mind. She wondered what she could do to make it go away.
When Julie couldn’t stand the aching any longer, she decided to take a break from running for a few days. Her hip flexor pain stopped, so she made the difficult decision of not running for two weeks.
Although it was painful to give up running, she hoped the pause would give the condition time to improve. And it did—until she hit the track again.
Just one minute into Julie’s first run in weeks, the pain surged back in full force. Frustrated, she decided to seek help.
What Didn’t Work
Julie started by exploring the typical healthcare route. But she quickly became irritated when her primary care doctor suggested rest and over-the-counter anti-inflammatory medications. She had already tried rest, to no avail, and she didn’t like the idea of medication. Her doctors thought she could have a labral tear in her hip, hip impingement or hip arthritis.
Unsatisfied, Julie searched for a better solution.
Her next stop was to see a physical therapist who was highly recommended by one of her friends. Physical therapy was covered by Julie’s insurance, minus deductible and copay, so she decided to give it a try.
01:15 Hamstring stretch with belt
03:26 Active Adductor stretch
05:25 Contract/ Relax Hip Capsule Stretch
07:28 Contract/ Relax Glute Stretch
09:29 90-90 Breathing
10:29 Glute Reach/ Rolls
13:05 Side Lying Isometric Adductor Presses
15:04 Hardstyle Planks
16:04 Split squats
44
views
Unlock Groin Pain Freedom with These 2 Simple Exercises!
Want more info?
Option 1: Groin On-Demand Webinar https://bit.ly/37thtNF
Option 2: Video Guide https://bit.ly/33aLIqC
Option 3 (the best): Work With Us https://www.p2sportscare.com/
To work with us, contact us using this link https://bit.ly/3zCBnzZ or call us 714-502-4243. We have online programs, virtual and in-person options.
Costa Mesa, CA www.p2sportscare.com
[Performance Place website low back article excerpt] Hip flexor pain can wreak havoc on your love for running. Many of us run for weight loss or because it’s something we feel we “need to do” to be healthy. But not Julie. She simply loved the act of running!
A 10-minute marathon runner in her mid-40s, Julie would typically run five days per week. Some days she would run in track groups, rising to the challenge when her friends motivated her to get faster. Other times, she relished the solitude of solo runs.
Running was Julie’s “fix.” So when a cluster of symptoms started keeping her from doing what she loved, she knew she needed to take action. She came to Performance Place® Sports Care after seven months of unsuccessful attempts at treating the pain. I knew a detailed examination and proper guidance on how to decrease her symptoms would get her on the right track.
How It All Started
About 10 months ago, Julie began to notice hip flexor and sit bone pain when she ran. Since she didn’t do anything to create it, she thought it would go away on its own—just like most of her minor running-related issues had in the past.
But this time was different.
Soon, her hip flexor and sit bone were starting to ache at the very first step of her morning run, causing her pain for the entire duration. Her sit bone region would feel aggravated all day, especially exacerbated when she sat for long periods of time at work. The pain weighed on Julie’s mind. She wondered what she could do to make it go away.
When Julie couldn’t stand the aching any longer, she decided to take a break from running for a few days. Her hip flexor pain stopped, so she made the difficult decision of not running for two weeks.
Although it was painful to give up running, she hoped the pause would give the condition time to improve. And it did—until she hit the track again.
Just one minute into Julie’s first run in weeks, the pain surged back in full force. Frustrated, she decided to seek help.
What Didn’t Work
Julie started by exploring the typical healthcare route. But she quickly became irritated when her primary care doctor suggested rest and over-the-counter anti-inflammatory medications. She had already tried rest, to no avail, and she didn’t like the idea of medication. Her doctors thought she could have a labral tear in her hip, hip impingement or hip arthritis.
Unsatisfied, Julie searched for a better solution.
Her next stop was to see a physical therapist who was highly recommended by one of her friends. Physical therapy was covered by Julie’s insurance, minus deductible and copay, so she decided to give it a try.
Under her physical therapist’s guidance, Julie tried to remedy her problems with a daily 15-minute routine consisting of stretching, glute strengthening and hip mobility drills. As her inpatient care, she received tool-assisted soft tissue work. But despite two months of diligently following this plan, her sit bone was still tender while sitting at work. And she still hadn’t returned to running.
Frustrated by the lack of progress, Julie continued searching for a real solution.
Next, she visited a chiropractor suggested by a friend whose sciatica and hip pain had improved under his care. Julie received adjustments and soft tissue work two times per week, which was covered partially by her insurance. But after three months, she saw little improvement.
At this point, Julie was beyond frustrated. It had been five months since she was able to run, and there was still no real solution in sight. She decided to search the Runner’s World forum for more ideas on how to loosen up her hip flexor. After learning about the Active Release Technique, she visited a specialist who cost $150 per 15-minute session—not a penny covered by her insurance. After two months, the treatment yielded no improvement.
#UnlockGroinPain #california
27
views
Sports Hernia Vs Inguinal Hernia - What is the Difference?
We'll be discussing the differences between sports hernia & inguinal hernia. Examination and testing for the groin, hip and lower abdominal region can help confirm a diagnosis (and rule out hip impingement, groin strains, and labral tears.
If you've ever been injured whilst playing sport, then you may be wondering what the difference between sports hernia and inguinal hernia is. We'll discuss the symptoms and differences between these conditions, and explain the treatments available. If you're ever in doubt about your injury, be sure to watch this video to find out more!
In this video, we're going to be discussing the difference between a sports hernia and a Groin Strain. We'll also be giving you some tips on how to tell the difference and what to do if you experience either of these injuries.
If you're looking for advice on how to treat a Sports Hernia or Groin Strain, then this video is for you! We'll discuss the symptoms and treatment options for each injury, and help you make the right decision for your health. We hope you find this video helpful!
Option 1: Groin On-Demand Webinar https://bit.ly/37thtNF
Option 2: eBook Unveiling The Mystery Behind Groin Pain in Athletes https://www.p2sportscare.com/product/understanding-sports-hernias-unveiling-the-mystery-behind-groin-pain/
Option 2: Video Guide https://bit.ly/33aLIqC
Option 3 (the best): Work With Us https://www.p2sportscare.com/
#sportshernia #abdominal #hippain
Sports Hernia Diagnosis
What Is A Sports Hernia?
A sports hernia is tearing of the transversalis fascia of the lower abdominal or groin region. A common misconception is that a sports hernia is the same as a traditional hernia. The mechanism of injury is rapid twisting and change of direction within sports, such as football, basketball, soccer and hockey.
The term “sports hernia” is becoming mainstream with more professional athletes being diagnosed. The following are just to name a few:
Torii Hunter
Tom Brady
Ryan Getzlaf
Julio Jones
Jeremy Shockey
If you follow any of these professional athletes, they all seem to have the same thing in common: Lingering groin pain. If you play fantasy sports, this is a major headache since it seems so minor, but it can land a player on Injury Reserve on a moments notice. In real life, it is a very frustrating condition to say the least. It is hard to pin point, goes away with rest and comes back after activity, but is hardly painful enough to make you want to stop. It lingers and is always on your mind. And if you’re looking for my step-by-step sports hernia rehab video course here it is.
One the best definitions of Sport hernias is the following by Harmon:
The phenomena of chronic activity–related groin pain that it is unresponsive to conservative therapy and significantly improves with surgical repair.”
This is truly how sports hernias behave in a clinical setting. It is not uncommon for a sports hernia to be unrecognized for months and even years. Unlike your typical sports injury, most sports medicine offices have only seen a handful of cases. It’s just not on most doctors’ radar. The purpose of this article is not only to bring awareness about sports hernias, but also to educate.
Will you find quick fixes in this article for sports hernia rehab?
Nope. There is no quick fix for this condition, and if someone is trying to sell you one, they are blowing smoke up your you-know-what.
Is there a way to decrease the pain related to sports hernias?
Yes. Proper rehab and avoidance of activity for a certain period of time will assist greatly, but this will not always stop it from coming back. Pain is the first thing to go and last thing to come. Do not be fooled when you become pain-free by resting it. Pain is only one measure of improvement in your rehab. Strength, change of direction, balance and power (just to name a few) are important, since you obviously desire to play your sport again. If you wanted to be a couch potato, you would be feeling better in no time. Watching Sports Center doesn’t require any movement.
Why is this article so long?
There is a lot of information on sports hernias available to you on the web. However, much of the information is spread out all over the internet and hard for athletes to digest due to complicated terminology. This article lays out the foundational terminology you will need to understand what options you have with your injury. We will go over anatomy, biomechanics, rehab, surgery, and even the fun facts. The information I am using is from the last ten years of medical research, up until 2016. We will be making updates overtime when something new is found as well. So link to this page and share with friends. This is the best source for information on sports hernias you will find.
Common Names (or Aliases?) for Sports Hernias
Sportsman’s Hernia
Athletic Pubalgia
Gilmore’s Groin
How Do You Know If You Have A Sports Hernia?
25
views
4 BEST Exercises For Pinched Nerve In Lower Back Nerve Pain
In this video, we will show the 4 best exercises for pinched nerve in lower back. These exercises and stretches work very well for lower back pain from disc herniations, pinched nerves, sciatica, SI joint, facets, muscle spasms, stiff lower back and even arthritis. Back pain with twisting, bending over, sitting and walking may all feel better with these exercises.
UPDATED VERSION OF THIS VIDEO HERE https://youtu.be/D3XbLT0d9IA
Want more info? We have a free webinar that covers the different types of low back pain you may be trying to fix. We cover disc herniations, pinched nerves, sciatica and even disc degeneration (arthritis) in extreme detail in this webinar. Use this link to get access. https://bit.ly/3zZ9Vgc
To work with us, contact us using this link https://bit.ly/3zCBnzZ or call us 714-502-4243. We have online programs, virtual and in-person options.
Costa Mesa, CA www.p2sportscare.com
[Performance Place website low back article excerpt] In this article (updated in 2021), I will be covering right and left side lower back pain. At the end of the article, it also covers the baffling situation of when your lower back pain CHANGES SIDES.
I’ll also be covering possible diagnoses, causes, and treatment options for single-sided lower back pain. This article will not cover sciatica in-depth (pain past the knee), but you can read all about that in one of my other articles here.
I’m Sebastian.
I’ve had lower right back pain and have been able to recover from it entirely. When I was 15, I was told I would need back surgery to reduce my pain so I could play baseball again.
Long story short, I did not require surgery, injections, or medication to return to baseball. I am 38 now and play baseball two days a week, lift weights, sprint, and have no issues with my lower back holding me back from doing what I want.
I’m telling you my story of recovery to let you know that you can recover as well (if you find the right person to help you as I did).
Hopefully, this article gives you better information to discuss with your sports chiropractor, physiotherapist, physical therapist, personal training, orthopedic or medical doctor.
Not everyone will get back to feeling 100%. As a general rule, the longer you’ve had it, the more challenging it can be. But this does not mean it’s impossible to feel physically capable again.
Let’s get on to the article.
Cause #1: Driving With Lower Right Back Pain
Driving your car is the #1 cause of single-sided lower back pain in people over 25.
If you are living in the US, you may experience more right-side low back pain when driving.
If you are in Europe, you may experience more pain in the lower left back while driving.
Why?
It has to do with the gas pedal.
As we discuss single-sided low back pain in this article, it may be helpful first to understand that not all low back pain is created equally.
Different causes for back pain have other mechanics, positions, and postures that will increase or decrease your pain.
I say this because if you’re in the US and you experience left low back pain while driving, that’s common as well. Keep reading this article.
As we venture into other causes of 1 sided low back pain, you’ll start to realize that positions and postures of your whole spine, arms, and legs matter. What you are doing with your body daily matters.
Now that you understand that postures and positions matter, you should realize that you also have some control over your condition. As I describe these mechanics, consider reversing them and seeing if it helps tomorrow. Not all ergonomic corrections yield immediate relief.
Back to driving…
Suppose you are in the US, lower right back pain while driving occurs as you tension the sciatic nerve with every up and down on the gas pedal. This tends to happen more in stop-and-go traffic. You may think it is the stress of the traffic, but that may not be so!
Multiple spinal nerve roots create your sciatic nerve that exits from tiny holes in your spine called intervertebral foramen. Your low back nerves could be subjected to pressure around this location, creating nerve swelling, making lower back stiffness and pain.
When you pressure a lumbar spinal nerve (L4, L5, or S1), typically stretching of the sciatic nerve will induce your lower back pain.
When you pressure a lumbar spinal nerve (L4, L5, or S1), typically stretching of the sciatic nerve will induce your lower back pain.
If this is you, simply move your seat closer to your steering wheel and increase the lumbar support on your chair (if you have one).
If you don’t have built-in lumbar support, roll up a towel and place it behind your lower back to let your lower back relax.
#ExercisesForPinchedNerveInLowerBack #pinchednerve #california
34
views
BEST Shoulder Blade Pain Relief Stretch On the Planet!
In this video, we will cover the best shoulder blade pain relief stretch. Shoulder blade pain can present under the shoulder blade or between the shoulders in the mid back. If this stretch works for you consider listening to our free audio on the biggest mistake people make when overcoming shoulder blade pain. Link here: https://bit.ly/2WyYNqo
#shoulderpain #neckpain #triggerpoint
Call: 714-502-4243 Costa Mesa, CA & virtual sessions
Web-based Rehab Guide for those ready to take action: https://bit.ly/3zF97Mo
Learn how to manage your flare ups and get through the day. Get right and make sure this nagging issue doesn't come back. We take everything we do at our clinic and share it with you in an easy to follow guide with video instructions on all exercises. Recovery might be simpler than you think!
Shoulder blade pain can feel like aches/spasms of muscles under the shoulder blade and are often confused as being muscle knots or trigger points. Shoulder blade pain is treatable with exercise therapy, in combination with manual therapy. Often times resolving in weeks to months, depending upon severity.
When we wrote this description, we decided to interview a few people just like you who’ve had shoulder blade pain. They were nice enough to share their stories so we can learn from them.
Case #1
The most enlightening of the interviews was Becky.
She was able to successfully return to full activity (work, yoga, and sleep) after suffering from shoulder blade pain just like you.
Becky has been a nurse for the past 10 years. She works 5 days a week in the hospital, moving patients, charting notes, and educating her patients about how to live a healthy life.
She’s now fully capable of rolling patients over in bed, pushing wheelchairs, and going throughout her day without neck, shoulder blade or arm pain. Sleeps like the dead at night without the assistance of medication of any kind.
But she didn’t always feel this good…
10 years ago, Becky was in grad school when she started to develop light headaches. Most days were mild just a light throbbing ache around the base of her head. Other days her headache would wrap around her head, towards her eyes and travel downward towards her shoulders. She got through most of the day with the help of a frequent self-massage and bi-weekly chiropractic work.
A few years later, her symptoms began to evolve.
Even though she feels great today, she can still recall the details like it was yesterday.
Most days she was in intense pain from the moment she opened her eyes in the morning. Sleeping was terrible due to the fact that it felt like someone was taking a hand drill and boring a hole into her right arm bone all night, directly through her bicep.
Throughout the day, her pain began to increase and creep down into her midback and upper trap area. The pain was so intense at times that she said she would have been “willing to cut her arm off” if it would take the pain away.
She had to stop doing yoga, was unable to sleep at night and considered quitting her job.
Tucking her chin and looking upward at the sky was painful. Looking down to her chest was much better, but still not pain-free. While driving, she could not turn her head to check for cars as she changed lanes. She even bought those little blindspot mirrors so she could safely change lanes.
Sounds intense right? Yet, she was able to overcome it.
What did she do to feel better?
She didn’t get better overnight. She spent months having her neck adjusted and getting massages with very temporary relief.
Eventually, she found a chiropractor specializing in focal soft tissue work help her release a nerve in her neck and shoulder. After that, she began to progressively get better. She looked forward to being able to work without pain and more importantly sleep and do yoga without any issues.
Want to be like Becky?
You can, you just need the correct plan of attack. The human body is truly resilient. You are just as resilient.
What is the correct plan of attack for shoulder blade pain?
Recovery is simple if we first address the red herring that tends to distract people away from REAL recovery.
REAL recovery returns you to ALL of the sports and hobbies that you love. Avoiding them because you feel “you’re getting too old” or afraid the pain will return is the wrong approach.
Ask yourself what REAL recovery is for you.
What activity would you return to if you had ZERO fear of your shoulder blade pain returning?
What would life be like without shoulder blade pain?
Set a goal and focus on it. Set your goals high.
Timecodes
0:00 - Intro To Neck And Shoulder Blade Pain
0:36 - Shoulder Blade Home Treatment Option 1
1:07 - Shoulder Blade Home Treatment Option 2
1:55 - Shoulder Blade Pain Anatomy
2:26 - Shoulder Blade Home Treatment Option 3
3:11 - Shoulder Blade Home Treatment Option 4
#ShoulderBladePainRelief #california
35
views
Shoulder Blade Neck Pain Relief (Deep Myofascial Release & Massage Therapy)
We perform deep tissue mobilization to release muscle spasms and provide pain relief for neck and upper shoulder blade pain on this woman. Active Release is the type of deep myofascial release we provide for our massage therapy.
Want more info?
Option 1: Shoulder Blade On-Demand Webinar https://youtu.be/W9irqQ1lIaM
Option 2: 12 Week Video Guide https://www.p2sportscare.com/product/shoulder-blade-pain-recovery-guide/
Option 3 (the best): Work With Us https://www.p2sportscare.com/
To work with us, contact us using this link https://www.p2sportscare.com/contact-form-youtube/ or call us 714-502-4243. We have online programs, virtual and in-person options.
Costa Mesa, CA www.p2sportscare.com
If you are dealing with a tightness in your mid-back / shoulder blade / traps area and it's not going away with stretching or massage, check out our audio file on the biggest mistake people make with shoulder pain.
Because we have gotten so many requests for exercises to do for shoulder blade and upper trap pain, we resorted to creating a very affordable guide. What should you do if this test worked for you? You should get this guide and see what else we know: https://bit.ly/31BQOvw ... or you can come see us in Costa Mesa, CA.
Shoulder blade pain can feel like aches/ spasms of muscles under the shoulder blade are often confused as being muscle knots or trigger points. Shoulder blade pain is treatable with exercise therapy, in combination with manual therapy. Often times resolving in weeks to months, depending upon severity.
As I wrote this article I decided to interview a few people just like you who’ve had shoulder blade pain. They were nice enough to share their stories so we can learn from them.
#NeckPainRelief #ShoulderBlade #california
17
views
2 Effective Treatments for One-Sided Headache Relief (You've Never Tried These!)
In this video, I'm going to show you two treatments for one-sided headache relief that you've never tried before!
UPDATED. VIDEO: https://youtu.be/yOlHoaqzJ-s
One of the treatments is a natural headache treatment that uses herbs and spices, and the other is a medication that you can take at home. Both of these treatments are effective and easy to use, so give them a try and see which one works best for you. After watching this video, you'll finally be able to relieve your one-sided headache pain!
#OneSidedHeadacheRelief #HeadacheRelief #california
Do you struggle with frequent one-sided headaches? Headaches are a complex topic, but if you have a tension headache, we have a few at-home remedies for you to try. The first exercise is to help lengthen the subocciptal muscles-try the chin tuck with rhythmic breathing to see if that helps! Dr. Dawne mentions that sitting up straighter can sometimes help you feel better immediately. The second at-home remedy to try is a soft tissue technique involving the head and neck region.
Dr. Dawne also suggests trying meditation and breathing exercises as a good at-home treatment for headaches! Give these a try and drop us a comment.
23
views
2 Most Common Causes Of Numbness & Tingling In Hand [Stretches & Exercises]
In this video we will explain the 2 most common causes Of numbness and tingling in the your hands and show the best stretch for hand numbness. In the beginning of the video we will cover why identification of the fingers involved is important. If you want more information we have a guide that covers all of this in MUCH more detail here www.p2sportscare.com/product/fix-hand-numbness/
If you would like help from us. Contact us! Call: 714-502-4243
Costa Mesa, CA & virtual sessions
Many people with hand numbness get told they have Carpal Tunnel, but the treatment for Carpal Tunnel often does not help their symptoms go away. Carpal Tunnel Syndrome is when the Median Nerve gets trapped under this area of the wrist called the Carpal Tunnel, which is covered by a thick, fibrous band called a Retinaculum, that covers the wrist like a bracelet. The Retinaculum can get thicker over time and in certain circumstances, which can compress the Median Nerve as it goes into the hand, causing Carpal Tunnel Syndrome. So if you have hand numbness and it's not Carpal Tunnel Syndrome, what could it be?
The doctors at Performance Place discuss the two most common reasons for hand numbness, which does not include Carpal Tunnel Syndrome. Yes, your Median Nerve may be irritated (or another nerve, depending on where the numbness in the hand exists). But it is more likely coming from the neck or somewhere higher up in the nerve than from down in the wrist area (such as the elbow or shoulder area). It is also possible that the primary issue is actually a disc injury in the neck, which is actually irritating the nerve that runs down into the hand. Many patients never even have the neck checked if they have hand numbness. Our approach is to look at every point along the nerve distribution for cause of the numbness. Numbness is always nerve-derived, the question is-where is the nerve being irritated and why?
These are questions we always seek to answer with our patients, and we attempt to teach you how to answer that question for yourself, using the tools in this video.
#CommonCausesOfNumbnessInHands #handnumbness #california
44
views
This is the World's BEST Stretch for Rhomboid Muscle Pain!
We're going to teach you the world's best stretch for rhomboid pain. This stretch will help to relieve shoulder blade pain and tightness in the rhomboid muscle.
If you're suffering from shoulder blade pain and rhomboid tension, then this is the stretch for you! By following this tutorial, you'll be able to relieve your pain quickly and easily!
Want more info? We have a great audio clip on why stretching is the biggest mistake people make when trying to recover from shoulder blade pain/ knots. This audio clip will cover trigger points, knots, scar tissue, spasms and nerve pain. Use this link to get access. https://bit.ly/3GaRKGe
#shoulderpain #midbackpain #triggerpoint
To work with us, contact us using this link https://bit.ly/3zCBnzZ or call us 714-502-4243. We have online programs, virtual and in-person options.
Costa Mesa, CA www.p2sportscare.com
Shoulder blade imbalance is very common both with shoulder symptoms, or without symptoms. Shoulder blade imbalance is when the shoulder blades are not even. One may be higher than the other, one might "wing", or one might be rotated more than the other. This is also known as SICK Scapula or Scapular Dyskinesis. Scapular Dyskinesis is when the scapula or shoulder blades do not move as they should, have poor stabilization, or are imbalanced in movement. It is slightly different than SICK Scapula because it does not involve movement.
We have received countless requests for exercises for shoulder blade and upper trap pain, so we created an affordable 4 week guide you can do from home.
If you're local, come see us in Costa Mesa, CA.
Shoulder blade pain can feel like aches/spasms of muscles under the shoulder blade and are often confused as being muscle knots or trigger points. Shoulder blade pain is treatable with exercise therapy, in combination with manual therapy. Often times resolving in weeks to months, depending upon severity.
When we wrote this description, we decided to interview a few people just like you who’ve had shoulder blade pain. They were nice enough to share their stories so we can learn from them.
Case #1
The most enlightening of the interviews was Becky.
She was able to successfully return to full activity (work, yoga, and sleep) after suffering from shoulder blade pain just like you.
Becky has been a nurse for the past 10 years. She works 5 days a week in the hospital, moving patients, charting notes, and educating her patients about how to live a healthy life.
She’s now fully capable of rolling patients over in bed, pushing wheelchairs, and going throughout her day without neck, shoulder blade or arm pain. Sleeps like the dead at night without the assistance of medication of any kind.
But she didn’t always feel this good…
10 years ago, Becky was in grad school when she started to develop light headaches. Most days were mild just a light throbbing ache around the base of her head. Other days her headache would wrap around her head, towards her eyes and travel downward towards her shoulders. She got through most of the day with the help of a frequent self-massage and bi-weekly chiropractic work.
A few years later, her symptoms began to evolve.
Even though she feels great today, she can still recall the details like it was yesterday.
Most days she was in intense pain from the moment she opened her eyes in the morning. Sleeping was terrible due to the fact that it felt like someone was taking a hand drill and boring a hole into her right arm bone all night, directly through her bicep.
Throughout the day, her pain began to increase and creep down into her midback and upper trap area. The pain was so intense at times that she said she would have been “willing to cut her arm off” if it would take the pain away.
She had to stop doing yoga, was unable to sleep at night and considered quitting her job.
Tucking her chin and looking upward at the sky was painful. Looking down to her chest was much better, but still not pain-free. While driving, she could not turn her head to check for cars as she changed lanes. She even bought those little blindspot mirrors so she could safely change lanes.
Sounds intense right? Yet, she was able to overcome it.
What did she do to feel better?
She didn’t get better overnight. She spent months having her neck adjusted and getting massages with very temporary relief.
Eventually, she found a chiropractor specializing in focal soft tissue work help her release a nerve in her neck and shoulder. After that, she began to progressively get better. She looked forward to being able to work without pain and more importantly sleep and do yoga without any issues.
Want to be like Becky?
You can, you just need the correct plan of attack. The human body is truly resilient. You are just as resilient.
#RhomboidMusclePain #california
31
views
4 BEST Lumbar Facet Syndrome Exercises For Pain Relief
Are you dealing with facet syndrome? If so, this video is for you! In this video, we'll show you some top 4 facet pain relief exercises that you can do at home to help relieve your symptoms.
If you're dealing with facet pain, then you need to watch this video! In this tutorial, we'll show you some top 4 facet pain relief exercises that you can do at home to help relieve your symptoms. Not only will these exercises help relieve your pain, but they'll also help improve your flexibility and range of motion!
#facetsyndrome #facetpain #lowbackpain
Want more info? We have a free webinar that covers the different types of low back pain you may be trying to fix. We cover disc herniations, pinched nerves, sciatica and even disc degeneration (arthritis) in extreme detail in this webinar. Use this link to get access. https://bit.ly/3zZ9Vgc
To work with us, contact us using this link https://bit.ly/3zCBnzZ or call us 714-502-4243. We have online programs, virtual and in-person options.
Costa Mesa, CA www.p2sportscare.com
[Performance Place website low back article excerpt] In this article (updated in 2021), I will be covering right and left side lower back pain. At the end of the article, it also covers the baffling situation of when your lower back pain CHANGES SIDES.
I’ll also be covering possible diagnoses, causes, and treatment options for single-sided lower back pain. This article will not cover sciatica in-depth (pain past the knee), but you can read all about that in one of my other articles here.
I’m Sebastian.
I’ve had lower right back pain and have been able to recover from it entirely. When I was 15, I was told I would need back surgery to reduce my pain so I could play baseball again.
Long story short, I did not require surgery, injections, or medication to return to baseball. I am 38 now and play baseball two days a week, lift weights, sprint, and have no issues with my lower back holding me back from doing what I want.
I’m telling you my story of recovery to let you know that you can recover as well (if you find the right person to help you as I did).
Hopefully, this article gives you better information to discuss with your sports chiropractor, physiotherapist, physical therapist, personal training, orthopedic or medical doctor.
Not everyone will get back to feeling 100%. As a general rule, the longer you’ve had it, the more challenging it can be. But this does not mean it’s impossible to feel physically capable again.
Let’s get on to the article.
Cause #1: Driving With Lower Right Back Pain
Driving your car is the #1 cause of single-sided lower back pain in people over 25.
If you are living in the US, you may experience more right-side low back pain when driving.
If you are in Europe, you may experience more pain in the lower left back while driving.
Why?
It has to do with the gas pedal.
As we discuss single-sided low back pain in this article, it may be helpful first to understand that not all low back pain is created equally.
Different causes for back pain have other mechanics, positions, and postures that will increase or decrease your pain.
I say this because if you’re in the US and you experience left low back pain while driving, that’s common as well. Keep reading this article.
As we venture into other causes of 1 sided low back pain, you’ll start to realize that positions and postures of your whole spine, arms, and legs matter. What you are doing with your body daily matters.
Now that you understand that postures and positions matter, you should realize that you also have some control over your condition. As I describe these mechanics, consider reversing them and seeing if it helps tomorrow. Not all ergonomic corrections yield immediate relief.
Back to driving…
Suppose you are in the US, lower right back pain while driving occurs as you tension the sciatic nerve with every up and down on the gas pedal. This tends to happen more in stop-and-go traffic. You may think it is the stress of the traffic, but that may not be so!
Multiple spinal nerve roots create your sciatic nerve that exits from tiny holes in your spine called intervertebral foramen. Your low back nerves could be subjected to pressure around this location, creating nerve swelling, making lower back stiffness and pain.
When you pressure a lumbar spinal nerve (L4, L5, or S1), typically stretching of the sciatic nerve will induce your lower back pain.
When you pressure a lumbar spinal nerve (L4, L5, or S1), typically stretching of the sciatic nerve will induce your lower back pain.
If this is you, simply move your seat closer to your steering wheel and increase the lumbar support on your chair (if you have one).
If you don’t have built-in lumbar support, roll up a towel and place it behind your lower back to let your lower back relax.
Moving your car seat forward allows for more knee bend (sciatic nerve slackening) and less pain.
72
views
The BEST way to Stretch Your Hip for Hip Flexor Bursitis Pain Relief
In this video, we're going to demonstrate the best way to stretch your hip to relieve hip flexor bursitis and hip joint pain.
This hip flexor stretch is a great way to improve your hip mobility and relieve hip joint pain. This is a great stretch for athletes, people who sit a lot, and anyone who has hip flexor pain. Give this stretch a try and see how it can help you relieve your hip flexor bursitis and hip joint pain!
#hippain #hipflexor #hipmobility
http://www.p2sportscare.com
714-502-4243 Costa Mesa CA
Option 1: Groin On-Demand Webinar https://bit.ly/37thtNF
Option 2: Video Guide https://bit.ly/33aLIqC
Option 3 (the best): Work With Us https://www.p2sportscare.com/
[Performance Place website low back article excerpt] Hip flexor pain can wreak havoc on your love for running. Many of us run for weight loss or because it’s something we feel we “need to do” to be healthy. But not Julie. She simply loved the act of running!
A 10-minute marathon runner in her mid-40s, Julie would typically run five days per week. Some days she would run in track groups, rising to the challenge when her friends motivated her to get faster. Other times, she relished the solitude of solo runs.
Running was Julie’s “fix.” So when a cluster of symptoms started keeping her from doing what she loved, she knew she needed to take action. She came to Performance Place® Sports Care after seven months of unsuccessful attempts at treating the pain. I knew a detailed examination and proper guidance on how to decrease her symptoms would get her on the right track.
How It All Started
About 10 months ago, Julie began to notice hip flexor and sit bone pain when she ran. Since she didn’t do anything to create it, she thought it would go away on its own—just like most of her minor running-related issues had in the past.
But this time was different.
Soon, her hip flexor and sit bone were starting to ache at the very first step of her morning run, causing her pain for the entire duration. Her sit bone region would feel aggravated all day, especially exacerbated when she sat for long periods of time at work. The pain weighed on Julie’s mind. She wondered what she could do to make it go away.
When Julie couldn’t stand the aching any longer, she decided to take a break from running for a few days. Her hip flexor pain stopped, so she made the difficult decision of not running for two weeks.
Although it was painful to give up running, she hoped the pause would give the condition time to improve. And it did—until she hit the track again.
Just one minute into Julie’s first run in weeks, the pain surged back in full force. Frustrated, she decided to seek help.
What Didn’t Work
Julie started by exploring the typical healthcare route. But she quickly became irritated when her primary care doctor suggested rest and over-the-counter anti-inflammatory medications. She had already tried rest, to no avail, and she didn’t like the idea of medication. Her doctors thought she could have a labral tear in her hip, hip impingement or hip arthritis.
Unsatisfied, Julie searched for a better solution.
Her next stop was to see a physical therapist who was highly recommended by one of her friends. Physical therapy was covered by Julie’s insurance, minus deductible and copay, so she decided to give it a try.
Under her physical therapist’s guidance, Julie tried to remedy her problems with a daily 15-minute routine consisting of stretching, glute strengthening and hip mobility drills. As her inpatient care, she received tool-assisted soft tissue work. But despite two months of diligently following this plan, her sit bone was still tender while sitting at work. And she still hadn’t returned to running.
Frustrated by the lack of progress, Julie continued searching for a real solution.
Next, she visited a chiropractor suggested by a friend whose sciatica and hip pain had improved under his care. Julie received adjustments and soft tissue work two times per week, which was covered partially by her insurance. But after three months, she saw little improvement.
At this point, Julie was beyond frustrated. It had been five months since she was able to run, and there was still no real solution in sight. She decided to search the Runner’s World forum for more ideas on how to loosen up her hip flexor. After learning about the Active Release Technique, she visited a specialist who cost $150 per 15-minute session—not a penny covered by her insurance. After two months, the treatment yielded no improvement.
In all, Julie’s seven months of health care had cost her more than $2500. But more critical than her financial hit was the void in her life from not running. She still couldn’t even jog without her hip flexor and sit bone immediately starting to ache.
Frustrated, stretched thin financially and still unable to do what she loved, Julie felt hopeless. She considered giving up running forever—until she found Performance Place® Sports Care.
127
views
How To Sleep Better With Sciatica: Find Relief Tonight!
In this video, we cover the most commonly asked questions about sciatica pain relief. The first question is Is Sitting Bad For Sciatica? The second is walking good for sciatica nerve pain? The third is laying down bad for sciatica? Sciatica is fixable without surgery or medication. We have whole Youtube series on sciatica pain relief
#sciatica #sciaticapainrelief #sciaticarelief
Sciatica is nerve pain in the back of the buttocks and leg (sometimes the calf and foot) which often increases with prolonged sitting, standing and walking.
Want more info? We have a free webinar that covers the different types of sciatica nerve pain you may be trying to fix. We cover sciatica in extreme detail in this webinar. Use this link to get access. https://bit.ly/3zZ9Vgc
To work with us, contact us using this link https://bit.ly/3zCBnzZ or call us 714-502-4243. We have online programs, virtual and in-person options.
Costa Mesa, CA www.p2sportscare.com
Dr. Gonzales & Dr Dawne of Performance Place deep dive into Sciatica. This video is for people who want to understand Sciatica very well. Sciatica is injury or irritation to the Sciatic Nerve, a long nerve that runs from your low back to your gluteal area all the way down to the calf and foot. It can feel like tightness or sharp pain or numbness and tingling. The Sciatic nerve is formed when several nerve roots coming out of the spine travel down the leg and come together to form a bigger nerve.
Often, there can be compression in the areas where it comes out of the spine, and that can cause the symptoms. Many activities can contribute to closing the bony hole that the nerve exits out of-causing compression. Some of these are daily activities like walking, or surfing. Activities with a large amount of spinal extension, or "arching" are the types of activities that keep these holes in their most closed positions, which can lead to other problems.
An Injury to a disc in the low back can also cause irritation or compression to the nerves that make up the sciatic nerve. The discs are little, "jelly-filled" pieces of tissue in between each vertebra and are right next to the spinal nerves that become the Sciatic. When the discs are injured, the "jelly" can move out of the disc and compress the nerve nearby. Different movements tend to injure the disc. Instead of extension or "arching" being a problem, the opposite movement is a problem. Bending forward, along with compression or rotation (turning) are the movements most likely to be injurious to a disc.
These two problems are the most common causes of Sciatica. To fix it, you must determine which of these two are your problem. There are some tests in this video to help you figure out which of the two is your problem and to help you differentiate from other diagnoses, such as Piriformis Syndrome. Piriformis Syndrome is one of the most common diagnoses confused with Sciatica.
Once you have determined what the primary cause of your Sciatica is, now you have to get rid of it. We have lots of videos about exercises for Sciatica or stretches for Sciatica that you can find on our channel. But the most simple piece of advice we can give for fixing this is: "Do What Feels Good". Remember, we are not looking for perfect, we are looking for progress.
There is a simple stretch demonstrated in this video that you can try today-and we discuss what you can do to keep it away in the long term. However you decide to treat this, make sure that you keep moving! The worst thing you can do for this condition is to let fear of movement get in the way of you physically moving your way to recovery.
Low back herniations, or lumbar herniations, are a very common injury we "fix" at Performance Place and they are the most common reason for sciatica leg pain. These injuries tend to follow similar patterns, and so we have decided to share two of the most common things that can help alleviate disc pain instantly.
Doctors Dawne and Sebastian spend some time talking about whether you can "fix" a disc or not, and what part MRI and imaging has to play in your recovery. They are the best at diagnosing the reason for your sciatica and helping you find sciatica relief quickly.
The Sciatic Nerve and Sciatica
The sciatic nerve is the large nerve of the body, composed of multiple spinal nerve root levels. It passes through the pelvis, under the hip external rotators (including the piriformis), through the hamstrings before splitting into two tributary nerves (tibial and common peroneal nerves).
The tibial nerve travels down the backside of the leg/ calf to the bottom of the foot. This branch is most commonly affected in sciatica. Sciatica in this region mimics plantar fasciitis, heel pain, metatarsalgia, and calf cramps.
TIMESTAMPS
00:00 Introduction
01:03 Why Does Sciatica Hurt More At Night?
07:40 How To Sleep With Sciatica?
184
views
Sciatica: Is Sitting or Walking Worse For Your Leg Pain?
Are you suffering from sciatica leg pain? In this video, we'll discuss the theory behind sitting and whether or not it's bad for leg pain. We'll also provide relief for sciatica pain with walk therapy.
If you're wondering if sitting is bad for sciatica, then this video is for you! We'll discuss the theory behind sitting and whether or not it's bad for leg pain. We'll also provide relief for sciatica pain with walk therapy. After watching this video, you'll know whether or not walking is the best way to relieve your sciatica pain!
Want more info? We have a free webinar that covers the different types of sciatica nerve pain you may be trying to fix. We cover sciatica in extreme detail in this webinar. Use this link to get access. https://bit.ly/3zZ9Vgc
#sciatica #sciaticapainrelief #sciaticarelief
To work with us, contact us using this link https://bit.ly/3zCBnzZ or call us 714-502-4243. We have online programs, virtual and in-person options.
Costa Mesa, CA www.p2sportscare.com
Dr. Gonzales & Dr Dawne of Performance Place deep dive into Sciatica. This video is for people who want to understand Sciatica very well. Sciatica is injury or irritation to the Sciatic Nerve, a long nerve that runs from your low back to your gluteal area all the way down to the calf and foot. It can feel like tightness or sharp pain or numbness and tingling. The Sciatic nerve is formed when several nerve roots coming out of the spine travel down the leg and come together to form a bigger nerve.
Often, there can be compression in the areas where it comes out of the spine, and that can cause the symptoms. Many activities can contribute to closing the bony hole that the nerve exits out of-causing compression. Some of these are daily activities like walking, or surfing. Activities with a large amount of spinal extension, or "arching" are the types of activities that keep these holes in their most closed positions, which can lead to other problems.
An Injury to a disc in the low back can also cause irritation or compression to the nerves that make up the sciatic nerve. The discs are little, "jelly-filled" pieces of tissue in between each vertebra and are right next to the spinal nerves that become the Sciatic. When the discs are injured, the "jelly" can move out of the disc and compress the nerve nearby. Different movements tend to injure the disc. Instead of extension or "arching" being a problem, the opposite movement is a problem. Bending forward, along with compression or rotation (turning) are the movements most likely to be injurious to a disc.
These two problems are the most common causes of Sciatica. To fix it, you must determine which of these two are your problem. There are some tests in this video to help you figure out which of the two is your problem and to help you differentiate from other diagnoses, such as Piriformis Syndrome. Piriformis Syndrome is one of the most common diagnoses confused with Sciatica.
Once you have determined what the primary cause of your Sciatica is, now you have to get rid of it. We have lots of videos about exercises for Sciatica or stretches for Sciatica that you can find on our channel. But the most simple piece of advice we can give for fixing this is: "Do What Feels Good". Remember, we are not looking for perfect, we are looking for progress.
There is a simple stretch demonstrated in this video that you can try today-and we discuss what you can do to keep it away in the long term. However you decide to treat this, make sure that you keep moving! The worst thing you can do for this condition is to let fear of movement get in the way of you physically moving your way to recovery.
Low back herniations, or lumbar herniations, are a very common injury we "fix" at Performance Place and they are the most common reason for sciatica leg pain. These injuries tend to follow similar patterns, and so we have decided to share two of the most common things that can help alleviate disc pain instantly.
Doctors Dawne and Sebastian spend some time talking about whether you can "fix" a disc or not, and what part MRI and imaging has to play in your recovery. They are the best at diagnosing the reason for your sciatica and helping you find sciatica relief quickly.
The Sciatic Nerve and Sciatica
The sciatic nerve is the large nerve of the body, composed of multiple spinal nerve root levels. It passes through the pelvis, under the hip external rotators (including the piriformis), through the hamstrings before splitting into two tributary nerves (tibial and common peroneal nerves).
The tibial nerve travels down the backside of the leg/ calf to the bottom of the foot. This branch is most commonly affected in sciatica. Sciatica in this region mimics plantar fasciitis, heel pain, metatarsalgia, and calf cramps.
TIMESTAMPS:
00:00 Introduction
01:42 Is Sitting Bad For Sciatica?
07:40 Is walking good for sciatica nerve pain?
10:21 Is laying down bad for sciatica?
218
views
Low Back Pain Twisting? DON'T Stretch & Rotate Like This (This Is How You Stretch Safely)
If you're suffering from low back pain, don't stretch, rotate and twist your low back like this! Instead, try these physical therapy stretches to help relieve your pain.
Low back pain is one of the most common injuries in the population, and it can be difficult to treat. In this video, I'm sharing with you some stretches that you can use to help relieve your low back pain. These stretches will help to improve your flexibility and relieve your pain, so don't try to stretch and twist your low back like this!
714-502-4243 | Costa Mesa, CA | http://www.p2sportscare.com
Part 1 Book: https://bit.ly/3G650fi
Part 2 Book (Diagnosis): https://bit.ly/3G6jxHZ
Part 3 Book (Treatments): https://bit.ly/3zBViPg
Part 4 Book (Weight Training): https://bit.ly/36kfHhH
Performance Place 12 Week Low Back Online Program: https://bit.ly/3F7HoWv
#lowbackpain #lowerback #lowbackpainrelief
[Performance Place website low back article excerpt] In this article (updated in 2021), I will be covering right and left side lower back pain. At the end of the article, it also covers the baffling situation of when your lower back pain CHANGES SIDES.
I’ll also be covering possible diagnoses, causes, and treatment options for single-sided lower back pain. This article will not cover sciatica in-depth (pain past the knee), but you can read all about that in one of my other articles here.
I’m Sebastian.
I’ve had lower right back pain and have been able to recover from it entirely. When I was 15, I was told I would need back surgery to reduce my pain so I could play baseball again.
Long story short, I did not require surgery, injections, or medication to return to baseball. I am 38 now and play baseball two days a week, lift weights, sprint, and have no issues with my lower back holding me back from doing what I want.
I’m telling you my story of recovery to let you know that you can recover as well (if you find the right person to help you as I did).
Hopefully, this article gives you better information to discuss with your sports chiropractor, physiotherapist, physical therapist, personal training, orthopedic or medical doctor.
Not everyone will get back to feeling 100%. As a general rule, the longer you’ve had it, the more challenging it can be. But this does not mean it’s impossible to feel physically capable again.
Let’s get on to the article.
Cause #1: Driving With Lower Right Back Pain
Driving your car is the #1 cause of single-sided lower back pain in people over 25.
If you are living in the US, you may experience more right-side low back pain when driving.
If you are in Europe, you may experience more pain in the lower left back while driving.
Why?
It has to do with the gas pedal.
As we discuss single-sided low back pain in this article, it may be helpful first to understand that not all low back pain is created equally.
Different causes for back pain have other mechanics, positions, and postures that will increase or decrease your pain.
I say this because if you’re in the US and you experience left low back pain while driving, that’s common as well. Keep reading this article.
As we venture into other causes of 1 sided low back pain, you’ll start to realize that positions and postures of your whole spine, arms, and legs matter. What you are doing with your body daily matters.
Now that you understand that postures and positions matter, you should realize that you also have some control over your condition. As I describe these mechanics, consider reversing them and seeing if it helps tomorrow. Not all ergonomic corrections yield immediate relief.
Back to driving…
Suppose you are in the US, lower right back pain while driving occurs as you tension the sciatic nerve with every up and down on the gas pedal. This tends to happen more in stop-and-go traffic. You may think it is the stress of the traffic, but that may not be so!
Multiple spinal nerve roots create your sciatic nerve that exits from tiny holes in your spine called intervertebral foramen. Your low back nerves could be subjected to pressure around this location, creating nerve swelling, making lower back stiffness and pain.
When you pressure a lumbar spinal nerve (L4, L5, or S1), typically stretching of the sciatic nerve will induce your lower back pain.
When you pressure a lumbar spinal nerve (L4, L5, or S1), typically stretching of the sciatic nerve will induce your lower back pain.
If this is you, simply move your seat closer to your steering wheel and increase the lumbar support on your chair (if you have one).
If you don’t have built-in lumbar support, roll up a towel and place it behind your lower back to let your lower back relax.
126
views
Best 3 Pillow Positions for Neck Pain Relief While Sleeping
Looking for a comfortable way to get relief from your neck pain during sleep? Look no further than the best pillow positions for neck pain relief! In this video, we'll show you three different comfortable pillow positions that can help you get a good night's sleep.
If you're experiencing neck pain, be sure to check out this video and try one of the best pillow positions for neck pain relief. With this information, you'll be able to get a good night's sleep and relieve your neck pain in no time!
#neckpain #tightneck #stiffneck
http://www.p2sportscare.com
714-502-4243 Costa Mesa CA
Option 1: Gift https://bit.ly/3f1JcWj
Option 2: Video Guide https://bit.ly/31BQOvw
Option 3 (the best): Work With Us https://www.p2sportscare.com/
[Performance Place website low back article excerpt] Nerd neck (aka Forward head posture) can be seen everywhere nowadays.
I personally hate the slang terms to describe someone’s physical state, but hey this is what people are searching!
In fact nerd neck is starting to go by other slang terms such as text neck, scholar neck, iHunch, iPosture, wearsie neck, computer neck, upper crossed syndrome, and dowager’s hump.
Who gets a nerd neck?
Teenagers, kids, and adults are all developing it.
This is not a problem only affecting certain ages and genders.
It primarily affects people who live a sedentary lifestyle. People who sit throughout the day tend to become affected more than those who are moving more throughout the day.
You could almost say that movement is the prevention of text neck!
We will cover this in sections to come.
Causes
Sorry I can’t help but interchanging the terms.
I think we can all point to a common theme. It’s screen time.
It does not matter what screen we are talking about. TVs, laptops, iPhones, Androids, iPads, Zoom, or Skype are offenders.
But we can’t only blame screen time.
Sitting time is just as bad, if not worse!
Poor sitting posture tends to endorse forward head posture, mid-back rounding (aka increased thoracic kyphosis), and lower back rounding.
Reversing these 3 spinal curves creates the perfect storm to create pain in the body, not just limited to the neck.
In the later section, I’ll cover symptoms more comprehensively.
Side effects of nerd neck
Direct side effects of nerd neck are:
local neck pain
headaches
pain between the shoulder blades
numbness of the hands
elbow pain
Some side effects of poor posture with sitting are:
lower back pain
hip or groin pain
glute ache
thigh numbness
leg pain
sciatica
knee pain
tight calf muscles
199
views
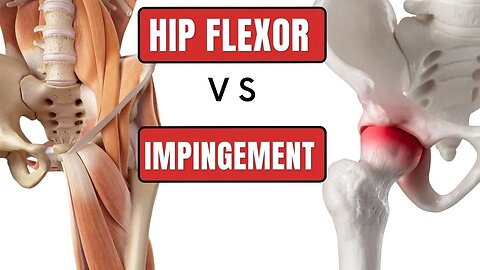














![2 Most Common Causes Of Numbness & Tingling In Hand [Stretches & Exercises]](https://hugh.cdn.rumble.cloud/s/s8/6/h/p/v/Y/hpvYp.oq1b.jpg)